Topics
01 - The first gynecological examination
Although usually scheduled as an “examination”, this first encounter with the gynecologist is often just a conversation. It is about building a trusting relationship and discussing issues that interest a girl or a young woman.
Be it about sexuality, contraception, vaccination or physical changes in the puberty, this first conversation is often an unplanned journey of discovery. If this first meeting is successful, it helps to build a positive attitude towards all gynecological examinations that come up in the future.


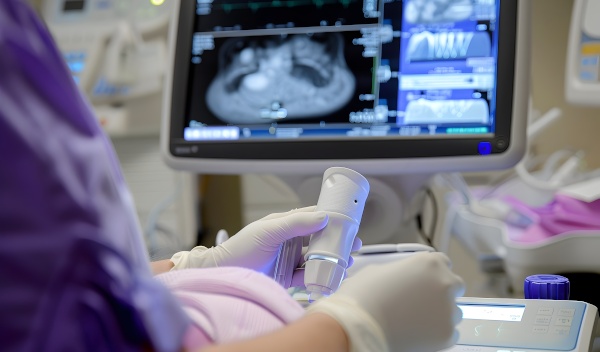
02 - Prenatal care
The development of a pregnancy is a natural process. In most cases, a pregnancy progresses without issues, but in some cases, problems may arise. The goal of prenatal care is to identify and address any issues that may occur during the pregnancy. Depending on the stage of the pregnancy, different aspects are focused on. In early pregnancy, the emphasis is on prenatal diagnostics and confirming the genetic health of the baby.
In the second half of pregnancy, the focus shifts to the metabolic health of both the mother and the unborn child, as well as detecting disorders such as gestational diabetes and high blood pressure. In the third trimester, attention is given to the growth of the baby and birth planning. The aim of prenatal care is always to provide care for both the mother and the child (or children in case of a multiple pregnancy). Depending on how the pregnancy progresses and any complications that may arise, the most suitable place for giving birth is also chosen.
03 - Prenatal diagnostics
Many years ago, when a woman was pregnant she didn’t know anything about what her child would be like. Only when the child was born, it became obvious whether the child was healthy or not. Nowadays it is possible to carry out various diagnostic tests early in the pregnancy and find out about medical conditions before the child is born. This possibility confronts pregnant women with several questions: Do I want to know everything about my child in advance? Are these tests necessary? What do I do if the test indicates a disease?
As the doctor in charge, I consider it my responsibility to talk about prenatal diagnostics in such a way that every pregnant woman understands the principles of the test and has exactly those tests done that she - or the couple - wants. Good information about prenatal diagnostics and the autonomy of the pregnant woman are the basis for all decisions.

04 - Birth Planning
Many years ago, when a woman was pregnant she didn’t know anything about what her child would be like. Only when the child was born, it became obvious whether the child was healthy or not. Nowadays it is possible to carry out various diagnostic tests early in the pregnancy and find out about medical conditions before the child is born. This possibility confronts pregnant women with several questions: Do I want to know everything about my child in advance? Are these tests necessary? What do I do if the test indicates a disease?
As the doctor in charge, I consider it my responsibility to talk about prenatal diagnostics in such a way that every pregnant woman understands the principles of the test and has exactly those tests done that she - or the couple - wants. Good information about prenatal diagnostics and the autonomy of the pregnant woman are the basis for all decisions.
05 - Healthy vaginal mucosa
Although, strictly speaking, it should be defined as "skin" (since there are no glandular exits), the term vaginal "mucosa" has become established because of its moisture, elasticity and sensitivity. The surface of healthy, normal mucosa in the vagina is colonized by numerous bacteria, usually called "vaginal flora" or "vaginal milieu". These bacteria largely responsible for the health and functioning of the vagina. A disturbed balance among different types of microorganisms leads to bacterial vaginosis, vaginal fungal disease or even inflammation in the vagina. Complaints such as itching, discharge, odor or pain are the most common reason for emergency visits to gynecological practices worldwide.
What can cause a disturbance in bacterial colonization? Stress, excessive washing, use of aggressive hygiene products, to name but a few. Gynecological examination and focused history-taking often reveal the cause of the complaints and can be used to work out a strategy for long-term vaginal health. Healthy, well-functioning vaginal mucosa is very important for overall gynecological health and a major contributing factor to satisfaction in sexual life.


06 - Menopause
By definition, menopause is the last naturally-controlled menstrual bleeding in a woman's life. In colloquial language, the word "menopause" is used as an umbrella term for the months before, during and after the end of menstrual bleeding. Due to hormonal instability, various physical and psychological changes become noticeable.
What is happening in my body? What will happen to me in the upcoming years? When will this phase be over? These are only some of the many questions that women ask themselves. Often there is a strong need to clear insecurities concerning the use of hormone replacement therapy. Am I allowed to, or do I have to take hormones? What are the benefits of hormone replacement therapy? What are the risks?
There are no generally right answers to these questions. In extensive discussion evaluating advantages and disadvantages of all possibilities, the needs and preferences of each individual woman can be met.
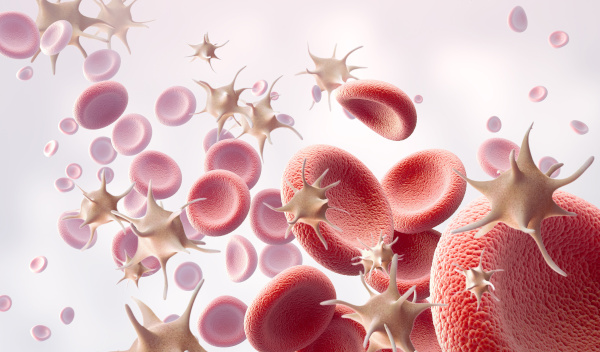
07 - PRP therapy (platelet-rich plasma)
In the PRP therapy, the patient‘s own blood is taken and centrifuged to isolate the platelet-rich plasma. This plasma contains a high concentration of growth factors and proteins that promote tissue healing and regeneration. The procedure is non-invasive. Since the plasma used is from the patient‘s own blood, allergic reactions are excluded. PRP therapy can be used in various areas where tissue regeneration is necessary: for treating wrinkles, stretch marks, injuries, vaginal atrophy, lichen sclerosus, hair loss, and many other conditions.
PRP has become firmly established, especially in the treatment of hair loss, and has been scientifically tested in many studies. In this treatment, the platelet-rich plasma is injected specifically into the scalp to stimulate the hair follicles and promote hair growth. Cell regeneration is stimulated, blood circulation to the scalp is improved and the hair follicles are strengthened. This can help slow down hair loss, thicken existing hair, and stimulate new hair growth.
The treatment is almost painless and does not require anesthesia. The number of sessions required may vary. However, at least 4 sessions every 2 weeks are recommended.

08 - Laser epilation: the most sustainable and gentle method of hair removal
Body hair has been removed differently through the centuries in different civilizations. The desire to reduce and modulate body hair is still current today. Different methods are used, These methods are not harmless and may cause severe side-effects such as burns or suffusions (hot and cold waxing), allergic reaction (chemical epilation) or local infection and bruising (shaving). All the above mentioned methods have in common that the body hair is not removed permanently but grows again, so that the desired hair-free condition cannot be achieved.
With Laser epilation, permanent hair removal can be achieved. It works on the principle of “thermokinetic selectivity”. During laser hair removal, the laser emits light that is absorbed by the pigment (melanin) in the hair. The light energy converts to heat, which damages the hair follicles. This damage inhibits future hair growth. White, light blonde and light red hair is unsuitable for treatment due to the lack of existing melanin. In our practice, laser epilation is carried out with the medical diode laser MedioStar. We treat armpits, legs and genital area.
The energy of the laser can only destroy hairs that are in the growth phase (about 20% of the total hair). Therefore, the treatment must be repeated several times. Avoid epilation, waxing and sun exposure before the treatment. We can provide counseling.



